Introduction
Radiographic images
Musculoskeletal X-ray films
Equipment and Procedures
Limitations
Fluoroscopy systems
Introduction
X-ray investigation is one the oldest and most commonly used radiological investigations in the medical field. It is essentially a painless radiological investigation.
X-rays are a form of electromagnetic radiation with higher frequencies and energy than visible light, microwaves and radiowaves. They are produced in an X-ray tube by focusing a beam of high-energy electrons on to a focal spot (tungsten) as target. From an X-ray tube, a small dose of these X-rays are emitted to pass through different parts of the human body. The transmitted X-rays pass on to an X-ray film placed inside a cassette (or a digital recording plate/detector), producing a visible image. Different film sizes are available for different parts of the human body.
When the transmitted X-rays reach the film cassette, a photochemical interaction occurs between the X-rays and a screen coated with a layer of the fluorescent particles. The X-rays can activate the fluorescent particles to emit light rays, which expose the photographic film, thus producing an image..Simply put, these transmitted X-rays can turn X-ray films black. The resulting images are commonly known as “X-ray” films (radiographs or plain films). Similarly, digital recording plate records signals upon X-ray exposure, and these signals are used for computing images.
Radiographic images
When a beam of X-rays passes through the human body, some are absorbed and some are scattered, reducing energy of the transmitted beam. As there are different types of tissues within our body, there are correspondingly different degrees of X-ray beam attenuation (reduction), producing images on the X-ray film. Tissues with low density, such as muscles, cause less X-ray beam attenuation than tissue with higher density, like bone, with the corresponding images appearing darker on the X-ray films.

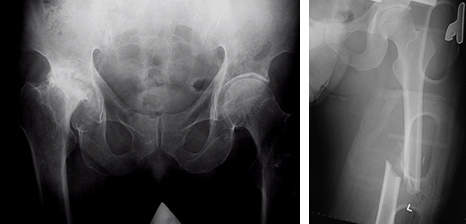
Musculoskeletal X-ray films
Depending on specific situations, your doctor may consider ordering plain films to help clinical diagnosis and management. A musculoskeletal X-ray film can give clear images of bones, including spine, shoulder, elbow, wrist, hand, pelvis, hip, knee, ankle and foot.
The following are examples of clinical conditions suitable for X-ray assessments:
managing trauma cases with bone fracture or joint dislocation
assessing and ensuring proper alignment of a fracture following a treatment
assisting orthopedic procedures, including fracture reduction, joint replacement or spinal surgery
evaluating medical conditions, including infection, degenerative arthritis, and abnormal bone growths
assisting the management of cancer
identifying and locating radio-opaque foreign bodies
identifying and locating radio-opaque loose bodies within a joint
detecting changes in bones and joints
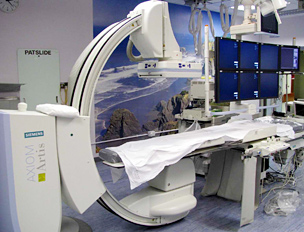
Equipment and Procedures
The X-ray equipment typically consists of an X-ray tube suspended over a table on which the patient lies. A drawer under the table can hold an x-ray film cassette (or a digital recording plate) of varying sizes, (or a digital recording plate/fixed detector), directly under the area of the body being imaged.
A radiographer will instruct you on correct body positioning when taking X-ray films. With proper setting of the X-ray machine and an X-ray film (or a digital recording plate/detector) of the appropriate size placed under the table in the area of interest, the radiographer then walks behind a control room to activate the X-ray machine. You must hold very still for a few seconds while the X-ray image is being taken. Tiny motion can result in blurred images.
You may be repositioned for another view and the process is repeated. Sometimes, an X-ray film may also be taken of the unaffected limb for comparison purpose, especially for paediatric patients with limb injuries.
The whole procedure usually takes about 5 to 10 minutes. You will then be asked to wait outside the X-ray room. The radiographer has to determine if the X-ray films taken are appropriate and high quality enough for clinical use.
The whole procedure is painless. You may experience discomfort from the cool temperature inside the X-ray room. With injury or pain, you may find holding still in a particular position or lying on the hard X-ray table uncomfortable. Your radiographer will assist you in finding the most comfortable position that can still allow proper X-ray imaging.
Limitations
Ususally, X-ray images provide little information about the soft tissues. In conditions that require a better assessment or delineation of soft tissues, other radiological investigations like Magnetic Resonance Imaging (MRI) or Ultrasonogram (USG) may be more appropriate. MRI may be more useful in identifying soft tissue injuries within the knee joint or shoulder joint. Ultrasound imaging, which uses sound waves instead of ionizing radiation, is useful for soft tissue injuries around joints.
Radiography use ionizing radiation. For women of reproductive age, radiation exposure of the abdomen and pelvis should be kept to a minimal.
Fluoroscopy systems
Fluoroscopy system refers to a technique of radiological examination of the anatomy and motion of internal structures by taking many continuous low-mA (milliamperes) or pulsed lighter mA images over a longer period of time. This allows real-time visualization of anatomic structures.
With low-mA X-rays, the fluorescing screen emits a faint light, which is amplified electronically by an image intensifier, and the images are usually viewed via a closed circuit television chain. Your orthopaedic surgeon may require the assistance of fluoroscopic examination during some parts of an orthopaedic surgery. Examples include reduction and/or fixation of fractures, placement of screws across sacroiliac joint in patients with pelvis fractures, placement of pedicle screws in spinal surgeries, and portal placement in minimally invasive spinal surgeries.
Other non-orthopaedic clinical applications include positioning for catheter placement, angiography, interventional radiology, dynamic studies such as swallowing examinations, as well as heart evaluations.
Dr. YU, Kong-san