Introduction
Musculoskeletal MRI
Equipment and Procedure
Hazards and precautions
Screen procedure before MRI scanning
Advantages
Limitations
Introduction
MRI stands for Magnetic Resonance Imaging, and is a non-invasive radiological investigation that does not use ionizing radiation (X-rays).
The patient is placed in an MRI scanner that generates a very strong magnetic field. Hydrogen nuclei in the body have a net magnetic movement and therefore behave like little magnets. These little magnets will then align themselves with the external magnetic field. Radiofrequency (RF) waves are then pulsed in, which scatter the hydrogen nuclei in all directions. Once the radiofrequency pulse is stopped, the hydrogen nuclei tend to realign themselves along the external magnetic field, but this happens at different rates in different tissues. Corresponding magnetic resonance (MR) signals are generated and recorded accordingly. These differential relaxation rates are used to create the MR images.
One advantage of MRI data over plain films (X-ray films) is that images can be obtained in any plane. Three basic planes used are axial, sagittal and coronal plane.
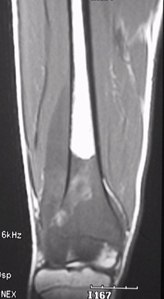
Musculoskeletal MRI
X-ray images provide little information about soft tissues. In conditions that require a better assessment or delineation of soft tissues, other radiological investigations, such as Magnetic Resonance Imaging (MRI), may be more appropriate.
MRI can be considered for detailed assessment of the following anatomical structures:
Synovial joints: shoulder, knee and hip
Soft tissues: muscles, tendons and ligaments
Spine
Examples of musculoskeletal conditions suitable for MRI are:
Knee joint: sports-related injuries such as anterior or posterior cruciate ligament tear, meniscus tear, and medial or lateral collateral ligament tear
Shoulder joint: rotator cuff syndrome, recurrent shoulder dislocation.
Spine: prolapsed intervertebral disc, cervical myelopathy, cervical trauma with neurological deficit
Work-related disorders caused by repeated strain, vibration or forceful impact
Infections: osteomyelitis, septic spondylitis
Staging of musculoskeletal tumors
Equipment and Procedure
The patient is placed within a large, powerful magnet, which produces a strong, external magnetic field. Hydrogen nuclei in the body align themselves with the external magnetic field. The body is then subjected to an impact of additional magnetic influences to derive magnetic resonance signals. A second magnetic field is then applied at right angles to the original external magnetic field. This field is applied at a specific frequency and is known as the radiofrequency pulse (RF pulse). The component of the net magnetisation vector in the transverse plan induces an electrical current in the RF coil, the MR signal. These MR signals obtained are then analysed by a computer and reconstructed mathematically into sectional images of the human body.
The MR signals depend on specific characteristics of the tissues and structures being studied. Also, by altering the duration and amplitude of the RF pulses, as well as the timing and repetition of its application, various imaging sequences can be employed to enhance image contrast, allowing identification and differentiation of different tissues, especially soft tissues.
Hazards and precautions
MRI involves the use of a strong magnetic field. Major hazard is related to the interaction with metallic materials and electronic devices.
Ferromagnetic materials within patients might potentially be “moved” by the strong external magnetic field during scanning, and can cause tissue damage. Examples include metallic fragments in the eye and some intracerebral aneurysm clips. In general, well-fixed orthopaedic metallic plates and screws pose no risk during scanning. Of course, safety of any individual device has to be confirmed before MRI scanning.
Patients implanted with medical electronic devices such as cardiac pacemakers, cochlear implants and neurostimulators should not be scanned.
Screen procedure before MRI scanning
Patients with the following conditions will be advised not to go through MRI scanning:
(i) any previous surgery with the use of metallic implant or electronic device
(ii) implanted cochlear device and cardiac pacemakers
(iii) presence of any metal foreign body
(iv) any possible occupational exposure to metal fragments
(v) any history of penetrating eye injury
(vi) allergy of gadolinium contrast medium
(vii) claustrophobia
If there is any doubt, your doctor can check with X-ray of the related area.
Advantages
The advantages of MRI include:
(i) not employing any ionizing radiation
(ii) images with excellent soft tissue contrast differentiation and characterisation
(iii) ability to obtain images in any desired plane
(iv) lack of artifact from adjacent bones
Limitations
Limitations of MRI include:
(i) high equipment costs, including both initial purchase and installation costs, and subsequent running and maintenance costs
(ii) patients with Claustrophobia may require sedation
(iii) not suitable for patients with cardiac pacemakers, metallic foreign objects, etc.
(iv)not as sensitive as CT in detecting small amounts of tissue calcification and acute haemorrhage
Dr. YU, Kong-san